Between Nov. 30 and Dec. 13, the number of people testing positive for influenza went from 13.5 per cent to 40.1 per cent, making it the highest increase since the start of Saskatchewan’s flu season.
According to the provincial government’s Community Respiratory Illness Surveillance Program (CRISP) Situation Report, which had a reporting period from Nov. 30 to Dec. 13, 2025, this also accounts for a higher rate than the past two time periods under the same time frame.
Read more:
- Sask. keeps COVID-19 vaccines free, unlike Alberta and Quebec
- Canada needs to invest in public health to regain measles elimination status
Dr. Joseph Blondeau, head of clinical microbiology at Royal University Hospital and the University of Saskatchewan, said the province has experienced a large amount of influenza A activity, especially in younger and older population groups.
“It’s resulted in an increase in visits to physicians or to emergency rooms, and even an increase in hospitalizations, and that’s been fairly uniform across the country,” said Blondeau, who is also the provincial lead for clinical microbiology.
He added that this includes admission into intensive care units.
“Sadly, we’re actually seeing this in the pediatric population as well. We always knew that there was a risk in elderly individuals — and that’s particularly true if you happen to be a person of advanced age and you have underlying medical conditions — then I think there’s even more of a concern about the possibility of having a severe infection,” Blondeau said.
According to the CRISP report, 99 per cent of the 2,245 flu detections since Aug. 24 have been influenza A (2,245). This includes subtypes like H3N2, which accounted for 67 per cent of detections (230).
One death was reported between Nov. 30 and Dec. 13.
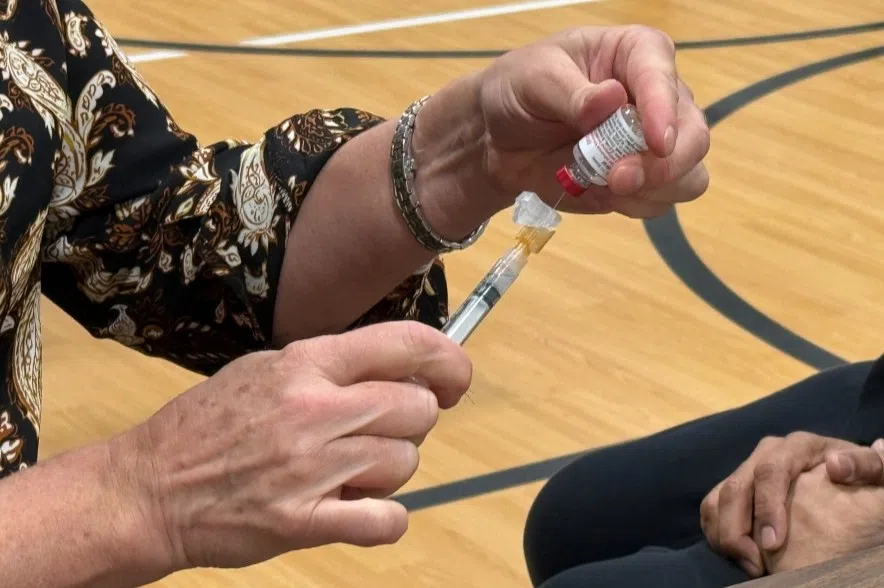
Blondeau advocated for people to get vaccinated as a means of protecting themselves from the flu’s spread and staving off severe infections.
“We encourage people every year to get out and get the flu vaccine, because influenza is one of those viruses that can actually end up resulting in the death of a patient across all age groups,” he said.
“This year, there’s been a little bit of negativity around it because the match has not been absolutely perfect; however, there is data that are available that shows that the vaccination (gives) you some level of protection against the H3N2 strain, plus the other two strains that are in the influenza vaccine…
“I think that there’s a belief amongst health-care professionals that having at least a partial level of protection may not prevent you from catching a milder infection of influenza, but certainly goes some way to protecting you against more severe infection requiring hospitalization.
“I don’t know that we’ve peaked yet, but I still think there’s every bit a good reason if you can get out and get your flu vaccine booked in to get that done.”
Blondeau also said measures like handwashing, physical distancing and masking can help protect people if they believe they might be exposed to people with potential flu symptoms.
The next CRISP report is scheduled to be released on Jan. 5.
Respiratory syncytial virus on the rise
Although influenza A has been the leading respiratory virus. Blondeau also warned about the rise of respiratory syncytial virus (RSV).
RSV’s test positivity remained stable for the late November to early December report, but Blondeau said it generally becomes more prevalent in January and February.
“RSV can also cause severe infection in elderly patients and in patients with underlying medical conditions,” he said.
“So if you’re going to be talking to a health-care provider, you might want to ask them about the RSV vaccine and whether or not you’re a candidate for that as well.”
Read more: